If you’ve recently received a letter about a change to your prescription coverage, that’s not unusual. From time to time, updates are made to the plan’s formulary (drug list), and some medications may be replaced with preferred alternatives.
These changes are manageable—you just need the right information to navigate them effectively.
What Is a Formulary Change?
A formulary is a list of prescription drugs covered by your health plan. When updates occur, certain medications may move off the list and be replaced with clinically appropriate alternatives.
If you receive a notice, it means:
- Your current medication may no longer be covered, or
- A more cost-effective or clinically appropriate alternative is now preferred
In either case, the next step is simple: talk with your doctor about switching to the recommended alternative.
Please be assured that your copay on the recommended alternative will not be more expensive than your current medication, and may actually be cheaper.
What You Need To Do
If you’re impacted by a formulary change, follow these steps:
1. Review Your Letter
Your letter will let you know:
- Which medication is affected
- The preferred alternative your plan covers
2. Talk to Your Doctor
Discuss whether the alternative medication is right for you. Your doctor will need to write a new prescription for the updated medication.
3. Fill a 30-Day Prescription First
Your new medication will typically begin with a 30-day supply at any retail pharmacy.
4. Transition to a 90-Day Supply
After your first fill:
- Your doctor will write a new 90-day prescription
- You can fill it through:
- Rx90 retail pharmacies (like Walgreens, Costco, Walmart, and select others), or
- Birdi mail order pharmacy
Remember that you must access mail order prescription services through MedImpact.
Formulary Change Process at a Glance
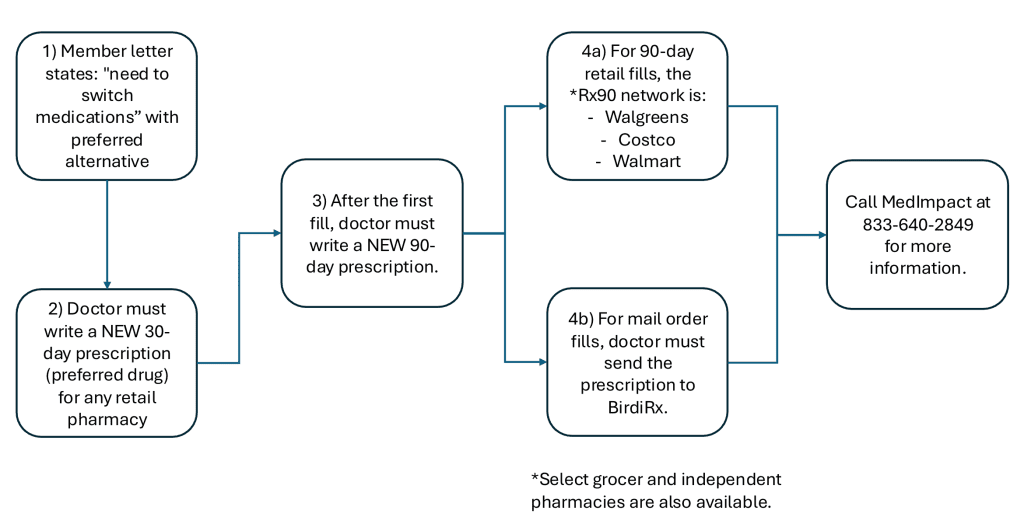
What If Your Prescription Is Denied?
Sometimes, when switching medications, you may run into issues at the pharmacy. If that happens:
- Ask for details – Your pharmacy can tell you why the prescription was denied
- Contact MedImpact/Elixir – They can help interpret the issue and guide next steps
- Talk to your doctor – They may:
- Adjust the prescription
- Recommend an alternative
- Submit a prior authorization if needed
Many issues—like refill timing or quantity limits—can be resolved quickly once identified.
How Are Formulary Changes Made?
Formulary updates are carefully reviewed by MedImpact’s Pharmacy and Therapeutics Committee, which includes physicians and pharmacists from a wide range of specialties.
They evaluate medications based on:
- Effectiveness
- Safety
- Quality
- Cost
- Potential side effects
This ensures that covered medications meet high standards for both clinical value and affordability.
We’re Here To Help
Formulary changes are designed to keep your prescription coverage safe, effective, and affordable. But we understand they can feel disruptive at first.
If you have questions or need help:
- Contact MedImpact Member Services: 833-640-2849
- Speak with your doctor or pharmacist for guidance
Please note that doctors’ offices are sometimes affected by delays. Taking action promptly—especially after receiving a letter—will help ensure you continue your medication without interruption.










